How do we Best Address Teen Vaping?
A public health emergency upends years of progress.
A public health emergency upends years of progress.

After years of seeing the number of teen smokers decline, the rise of e-cigarettes and vaping (inhaling and exhaling of vapor produced by an electronic device) is leading to a substantial increase in use by teens. What was initially touted as a healthier smoking cessation method for adults is having the opposite effect on teens.
Just this month, San Francisco became the first U.S. city to ban the sale of all e-cigarettes, and new laws went into effect in Colorado limiting e-cigarette and flavored tobacco use. Widespread concern over the impact on youth smoking have led to these legislative changes.
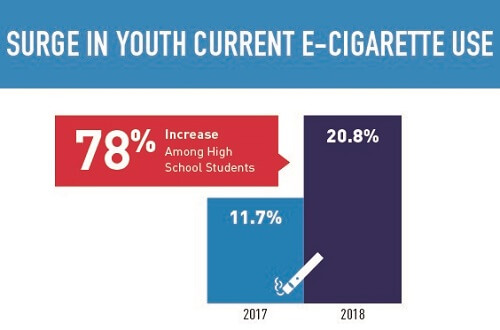
Source: FDA - 2018 National Youth Tobacco Survey results
Visit your local high school, and it’s obvious that teens are now vaping in record numbers. The 2018 National Youth Tobacco Survey, which is funded by the Center for Disease Control and Prevention and the Food and Drug Administration, shows e-cigarette use went up 78% for high school students between 2017 and 2018 alone.
Teens are now more likely to use e-cigarettes than other types of tobacco products. The Monitoring the Future survey, conducted by the University of Michigan, also found that nicotine use by high school students via vaping has nearly doubled.
Not all e-liquids or vape juice contains nicotine, but even without it e-cigarette aerosol can contain heavy metals and other potentially cancer-causing compounds. Nicotine exposure during adolescence has been shown to be harmful and even increase the risk of potential use of other substances. Vaping may also lead to conventional smoking, as National Institute on Drug Abuse has found that nearly a third of teen e-cigarette users begin smoking other tobacco products within six months.
These trends are alarming because for the decade prior, teen smoking had actually declined, thanks in part to the success of edgy public education campaigns, aggressive anti-smoking policies, and overall tobacco use losing the social cachet and acceptance it once had. Unfortunately, nearly 80% of youth were exposed to e-cigarette marketing in 2016 according to the latest information available from the CDC, and increased sales have outpaced medical research and knowledge of the near- and long-term health effects of prolonged use.
The National Safety Council has addressed the public health impact of cigarette smoking by recommending six specific tobacco control measures, and a new policy to address electronic nicotine delivery system, or ENDS products, calling for additional regulations and raising public health risk awareness.
Many communities have been overwhelmed by the influx of teens who vape at school. At the 2018 National Prevention Network conference, public health advocates shared that some schools are starting to ban USB’s, as teachers can’t tell the difference between Juul devices (the most popular e-cigarette manufacturer on the market) and flash drives.
Media reports have indicated that schools go to extreme lengths to curtail use, such as limiting bathroom access, banning certain types of clothing that could be used to hide vaping devices, randomly testing students for nicotine, punishing fines and police involvement. Some schools also are looking beyond short-term penalties towards shifting culture through awareness, public education campaigns and community outreach.
There’s more we can do to eliminate disparities in how we regulate tobacco products, regardless of their delivery system. So far, 14 states have raised the minimum age of sale for tobacco products to 21. Legislation also has been introduced requiring child-resistant packaging for liquid nicotine containers, aiming to reverse an upward trend of accidental ingestion of e-liquids by children that were reported to U.S. poison control centers.
Nearly nine out of 10 cigarette smokers first try cigarette smoking by age 18, so reducing exposure to youth is key to preventing future health impacts. Prevention can happen at home, with parents and caregivers talking with teens about e-cigarettes; at work, by expanding smoke-free policies to include electronic nicotine delivery system (ENDS) products; and in our communities, by restricting use, sales and advertising to decrease exposure to young people.
With a century-long legacy, the National Safety Council is a global center for safety expertise. Let's work together to align resources. We look forward to learning about ways we can join efforts to expand safety everywhere!
There are no items in your cart